Addressing this year’s High Commissioner’s Dialogue on Protection, Raouf Mazou, shines a spotlight on the need for inclusion when it comes to health policies.
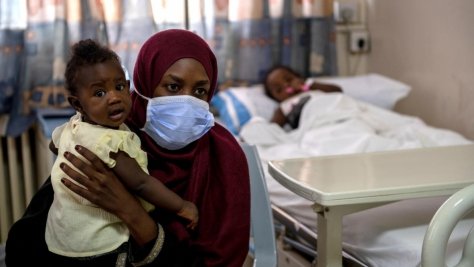
Sudanese refugee Ekram Yacoub's three-year-old daughter Rana (right) has health problems that require regular admission at Luzmila Hospital. Her healthcare costs are covered by UNHCR. Ekram, 30, arrived in Jordan in May 2016.
“We all know the principle of leave no one behind and it is clear that the inclusive national policies and services will contribute towards achieving universal health coverage for all,” said Raouf Mazou.
Addressing a session in the High Commissioner’s Dialogue focused on Resilience and Inclusion in Health, Mazou said that at least 85 per cent of refugees and displaced people are hosted in developing countries. He noted that this put pressure on health systems even before the COVID-19 pandemic struck this year.
“It is not only refugees who benefit.”
“What we have also heard from many of the representatives of government who joined us today is the willingness of a number of states to better include refugees into national health services,” he said, adding that states require support to achieve this.
“It is not only refugees who benefit from comprehensive responses … refugee-hosting countries themselves can benefit from inclusive approaches,” he said. Host countries can benefit from development funding for both refugees and hosts and from the skills and labour that refugees can contribute to society.
The forum, which brought together experts, academics, government leaders and health professionals, looked at both emergency responses and longer-term approaches. Nigel Pearson acted as moderator and the event included contributions from several people directly involved with implementing health care plans in individual countries.
Fezzeh Hosseini, 38, is a doctor and Afghan refugee in Iran’s Esfahan province who heads a team of doctors and nurses. Since the pandemic began, she has worked to ensure that both Iranians and Afghan refugees have information and access to health services.
She said many refugees struggled to find employment and so could often not afford to access health services.
“The message I’m trying to get through is to get as much international help to support health services for Iranians and Afghans alike,” she said.
“Host communities near to the refugees have free access.”
Alfred Driwale, Uganda’s Assistant Commissioner for Health Services, said refugees in his country had access to health care and could also work and this helped everybody in the long run.
“Because of that integration, host communities near to the refugees have free access through third party partners,” he said.
Akramul Islam, director of the communicable diseases and water, sanitation and hygiene (WASH) programme at BRAC, an international development organization in Bangladesh, said his organization had worked with partners including UNHCR in measures to prevent and treat diseases such as malaria, tuberculosis and HIV.
When the pandemic began, the organizations had provided education, training and healthcare to prevent its spread among Rohingya refugees, he said.
The high-profile Dialogues were established to promote an exchange of views between refugees, governments, civil society, the private sector, academics and international organizations on emerging challenges in humanitarian protection.
This year the sessions are being held virtually over seven weeks – with a focus on how the COVID-19 pandemic affects displaced and stateless people.
Μοιράσου το στο Facebook Μοιράσου το στο Twitter