Never a quiet day in Bunj Hospital maternity ward

Never a quiet day in Bunj Hospital maternity ward
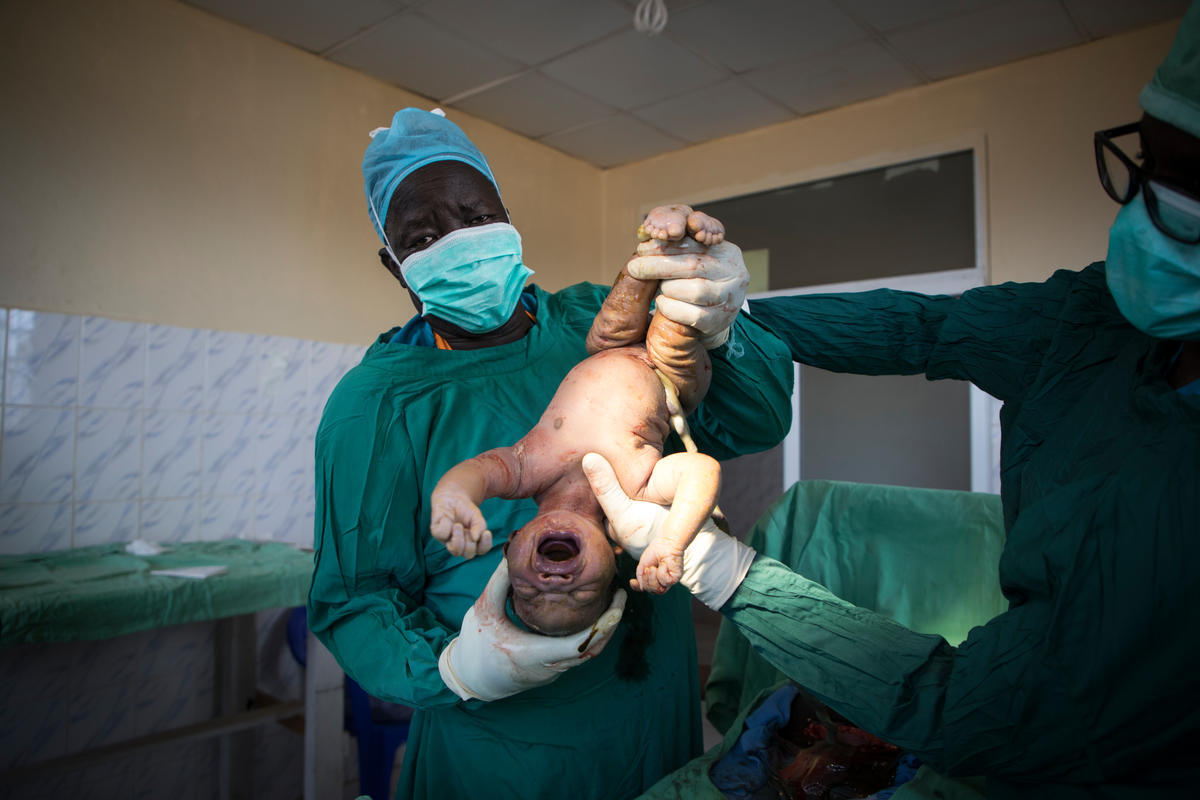
There is never a slow day at the maternity ward in Bunj Hospital in South Sudan. Some women walk in, but most arrive by ambulance or are carried at shoulder height on rope beds.
Gisma Al Amin, 28, a Sudanese refugee, arrived after a bumpy 40-minute ambulance ride from the refugee camp where she lives. Within hours, she was holding a baby boy, her fifth child and her third caesarian delivery. She named him Atar, after the doctor who delivered him.
“I had heard of Dr, Atar when I still lived in Blue Nile,” Gisma said, referring to the state in Sudan that she fled in 2013, when her village was attacked by armed groups.
“Many people talked about him there. Everyone knows that he gives very good care. If you ask people in Blue Nile, they will say, ‘He is our doctor’.”
Evan Atar Adaha (he goes by his middle name) is a South Sudanese doctor who spent 12 years working in Kurmuk in Blue Nile, often as the only surgeon.
He, too, fled fighting in 2011 with tens of thousands of Sudanese. He is now the chief surgeon and medical director at the Bunj Hospital, close to the border with Blue Nile.
“It is necessary for me to understand what stresses the patients are going through.”
The 120-bed hospital is the only functional surgical facility in Upper Nile State and it now includes a neonatal section and a 20-bed tuberculosis ward. Open 24 hours a day, it serves a population of almost 200,000, including 144,000 refugees.
Health-care facilities in the refugee camps are linked with Bunj Hospital.
On average, the surgical team of four doctors operates on 58 cases per week. In 2017, about 70 per cent of the surgical cases received were from refugee communities. There is no isolation ward and no intensive care.
When the wards get crowded and hot, many family members move the patients out on to the hard-packed earth of the hospital yard, where they cook on open fires under the rustling palms and neem trees, shooing away wandering goats, stray dogs and baby pigs.
Dr. Atar estimates that he must have delivered more than 800 babies since he arrived in Maban. It is common practice here for women to name children after the delivery doctor. The nurses joke that there are many little Atars growing up in Upper Nile and Blue Nile.
The maternity ward has eight beds but it can accommodate up to 20 cases. People are discharged within 24 hours after a normal delivery. One particularly busy night Dr. Atar performed six caesarian sections.
“You are a human being and therefore you can plan for your life.”
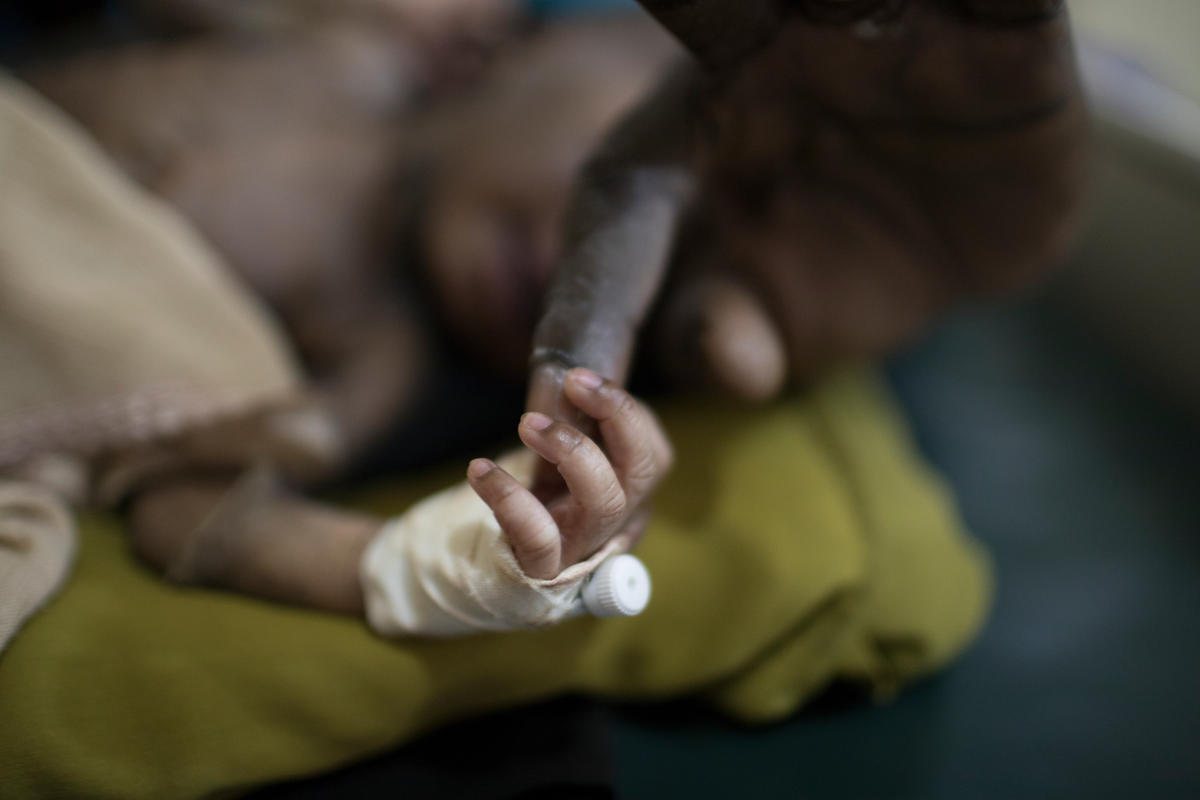
Gisma’s child had a skin infection and mother and son spent a few days in the ward. On his daily rounds, Dr. Atar would visit Gisma to talk about family planning and the risk of multiple caesarians, how every new one increases the risk to the life of mother and child.
Diplomatically, he suggested that her husband come to visit so that he could talk to both about the importance of family planning.
“It is necessary for me to understand deeply what the stresses are the patients are going through,” Dr. Atar says. “And when they tell you the secrets of their life, then you have the opportunity to advise them or to tell them what they should do.”
You have to be diplomatic, he adds, and let the husband see the advantage. “I tell the men: ‘If you are comfortable with the number of children, your wife should have a bilateral tubal ligation.
“All these children need to go to school. If you have so many, how can you send them all to school? The hen hatches maybe 20 chicks, but at the end of the day only five survive. You are a human being and therefore you can plan for your life’.”
Gisma needed no convincing. “I want my children to have an education,” she declared. “This boy will go to school to be a doctor.”