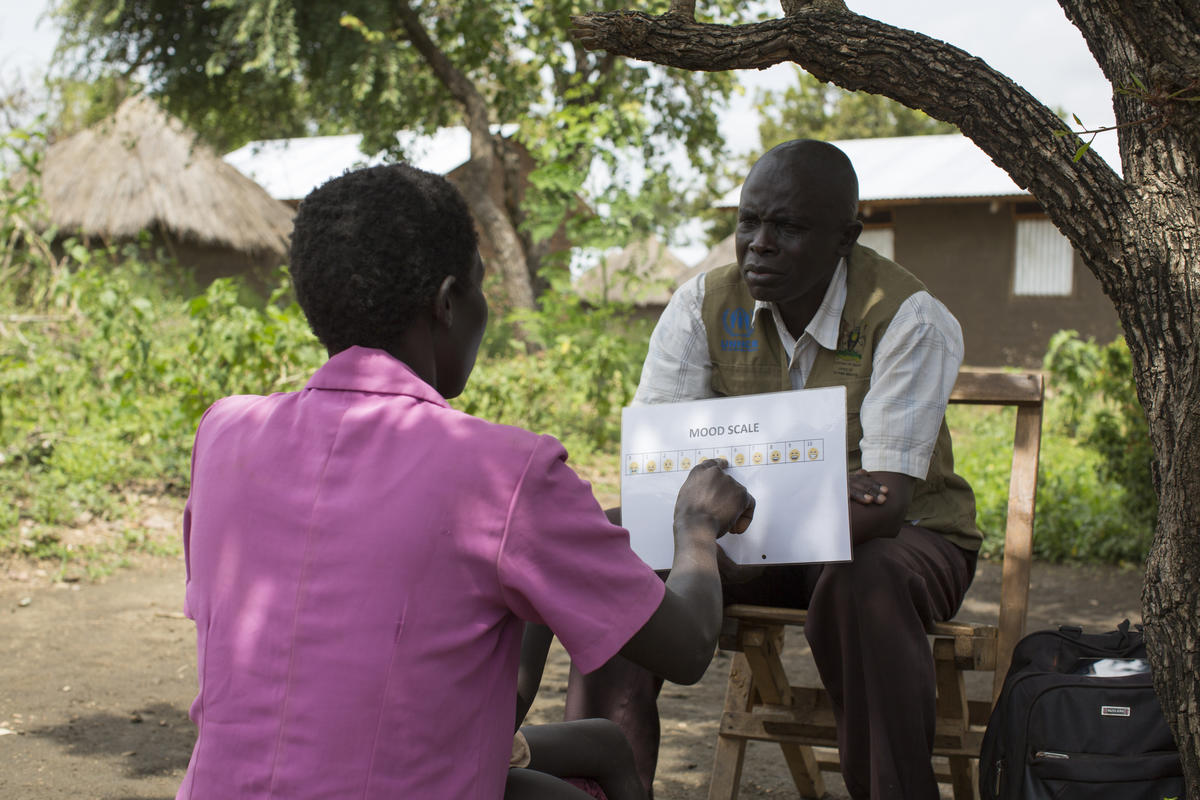Refugees deliver mental health services to locked down camps in Iraq

Refugees deliver mental health services to locked down camps in Iraq
Falak Selo knows what the sudden loss of home, country and loved ones can do to a person’s mental wellbeing. She was studying philosophy at the University of Damascus in 2013 when Syria’s civil war reached the area where her mother and sister were living.
She abandoned her studies to flee with them to the town of Akre in northern Iraq where a former prison for political dissidents during Saddam Hussein’s administration had been turned into a shelter for over 1,000 Syrian refugees.
“It was difficult, to cross borders and come to a country that is completely strange,” recalls Falak, who still lives in “the Citadel”, as Akre camp is locally known.
Accommodation in the fortress-like structure is cramped, with little natural light, but Falak has learned skills to help her cope, and, since 2017 she has been sharing them with other refugees at Akre through her role as a community worker with the UN Refugee Agency’s mental health and psychosocial support (MHPSS) unit.
“It’s a place where you see a lot of pain in people,” she says. “It gives me a feeling of fulfillment when I see that people are trusting me and coming back for my support.”
That support and intimate knowledge of the mental distress facing refugees in the camp are needed now more than ever. UNHCR has been receiving alarming reports of a surge in mental health issues among refugees and forcibly displaced people across the Middle East region, and beyond, since the onset of the coronavirus pandemic.
“While many refugees and internally displaced people are remarkably resilient… their capacities to cope are now being stretched to the limit,” warned UN High Commissioner for Refugees Filippo Grandi in a statement last month.
For refugees in Akre and eight other camps scattered across the Kurdistan Region of Iraq, the elevated levels of anxiety and depression stem less from fear of the virus itself than from the loss of income resulting from strict curfew measures that have prevented them from leaving camps to work in nearby towns and cities, community workers say.
“Most of the camp residents are daily workers and after years of displacement some of them felt that they had gained control of their lives,” explains Kawa*, a community worker and Syrian refugee living at Domiz 1 camp, near the city of Dohuk. “Now, with the loss of livelihoods, it feels for many people that they are passing through the same problems and shocks over and over.
"I won't be exaggerating if I say that everybody is afraid."
“Living in the camp, I can see how the situation is,” he adds. “Stress, worry and fear are widespread. I won’t be exaggerating if I say that everybody is afraid.”
The lockdown has also meant that psychiatrists and counsellors working for the MHPSS unit have had little or no access to the camps and have had to shift to providing counselling through helplines and phone consultations. Fortunately, community workers who live in the camps are still able to hold impromptu mental wellness sessions on their neighbours’ doorsteps, drawing on their training on psychological first aid.
“In our way of living, families tend to gather in front of their houses for chatting and having tea,” explains Kawa. “We are targeting these groups of people while ensuring physical distancing between us and them.”
Hivine Ali, a mental health and psychosocial support officer with UNHCR who coordinates with the team of 19 community workers, says their presence in the camps has helped the MHPSS unit continue delivering much needed mental health support during lockdown.
“We knew they were important before, but now the role of the community workers is even more important,” she says.
"We knew they were important before, but now the role of the community workers is even more important."
While group activities at schools and community centres have had to stop, the community workers are still running awareness sessions at primary health care centres, where they also put on personal protective equipment (PPE) to do one-on-one counselling. Their work does not stop there, says Falak.
“I’m following up on cases that need further care on a personal basis, because we are all neighbours in here. I am doing this during working hours and after working hours when the neighbours visit, and we chat over tea.”
People with pre-existing conditions that have become more severe since the onset of the pandemic, such as obsessive compulsive disorders, often need to be referred to psychiatrists and psychologists for more specialised care. But the community workers are able to help those suffering from stress, anxiety or depression through their training in a psychological intervention developed by the World Health Organization called Problem Management+ (PM+).
“We ask them what they did in previous times to cope,” says Hivine. “Refugees really have gone back to the previous coping mechanisms they had. They experienced being restricted to the camp when they first arrived, and now they’re trying to deal with this.”
When the main source of distress is a loss of income and inability to put food on the table, the community workers can refer cases to NGOs and UN agencies who can help with food or cash assistance.
For those the community workers cannot reach during lockdown, UNHCR has turned to a radio station based in Domiz 1 camp that broadcasts to local communities, including camp residents and internally displaced people. Every Wednesday, a clinical psychologist from UNHCR goes on air to share mental health tips and take calls from listeners.
Kawa says it is the only local programme he knows of that is dealing with the mental health consequences of the pandemic rather than its threat to public health.
Help is also available for the community workers themselves to ensure they are not over-burdened.
“We’re in contact with them on WhatsApp groups so we can see how things are, how they are,” says Hivine. “We make it clear that whenever they feel they need someone to talk to, we’re available.”
Kawa confirms that the self-care tips are “extremely helpful”.
“We need to help ourselves to help others,” he says.
*Asked that his last name not be used
Additional reporting and writing by Kristy Siegfried