With Syria refugee crisis, Lebanese health services improve
With Syria refugee crisis, Lebanese health services improve
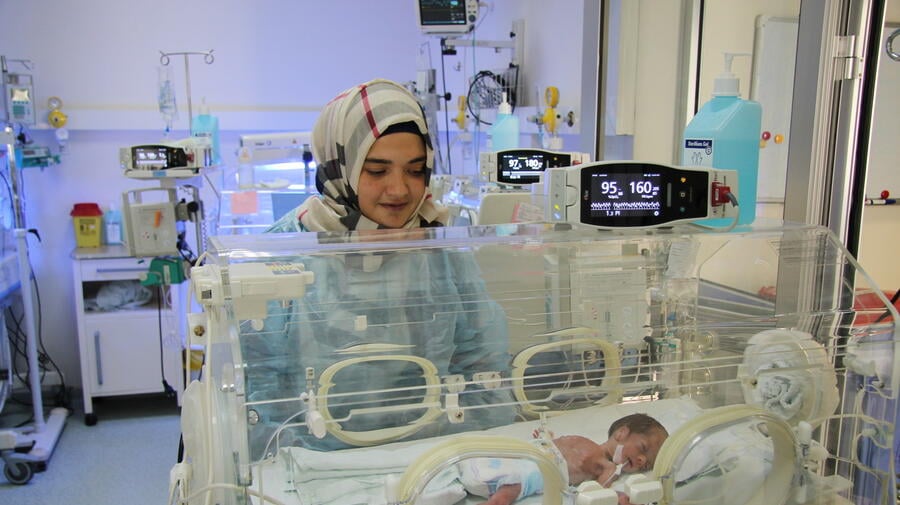
Lebanese mother Diana, 25, checks up on her baby at the Neonatal Intensive Care Unit at the Tripoli governmental hospital in northern Lebanon. The mother and baby are among beneficiaries of improved primary healthcare in Lebanon through funding from UNHCR.
TRIPOLI, Lebanon – Since the day she was married at 13 years of age, Ola,* a Lebanese woman, has never known safety. An abusive husband, a miscarriage and a series of psychological misdiagnoses left her on the edge of despair.
But following an unexpected turn of events, Ola, now 50, is finally receiving the expert mental healthcare treatment that she urgently needs. “I used to feel overwhelmed with fear,” she told UNHCR, the UN Refugee Agency. “Fear of everything and anything.”
She is among thousands of vulnerable Lebanese who have gained access to a full range of public primary healthcare services – from psychiatric help to neonatal and pediatric care - since the crisis in Syria next door led to a massive influx of vulnerable refugees.
After war broke out in Syria in early 2011, over one million refugees have sought safety in Lebanon. They are registered in country with UNHCR, which is working closely with the Ministry of Public Health to meet their needs.
With generous funding from donors, Lebanon has been able to integrate a range of much-needed services within primary healthcare centres (PHCs), benefiting both Syrians and poor Lebanese.
Prior to the crisis, the Hôpital Psychiatrique De La Croix – a charitable organization on the outskirts of the capital, Beirut – was the only accessible provider of mental healthcare services in the whole country, making support for those outside the capital, like Ola, especially hard.
" A closer look at the impact of the refugee crisis reveals a lesser-known reality."
Tonina Frangieh, a senior mental health and psycho-social support officer with the International Medical Corps in northern Lebanon, said mental healthcare was previously “unheard of” in the north of the country.
“In the past, mental health patients were dismissed as crazy or thought to be possessed;” she added, “they used to be beaten, locked up and sometimes even chained.”
Now, psychological help is among the many services that are more widely available with the gradual improvement of healthcare provision since the Syria crisis began.
“With the arrival of refugees, healthcare needs skyrocketed,” said Randa Hamadeh, head of the primary healthcare department at Lebanon’s Public Health Ministry. “With generous support from the European Union, we worked with UNHCR and integrated mental health, malnutrition treatment, and reinforced reproductive healthcare services within the primary healthcare system nationwide.”
As a result, Lebanese and Syrian patients now have access to completely free-of-charge vaccinations with support from UNICEF and WHO. Even the vaccine-related consultation fee that used to apply prior to the crisis has been waived.
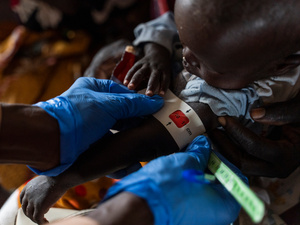
From the outset, primary healthcare centre staff have received training in effective vaccine management, and other key services such as the diagnosis and treatment of malnutrition and the clinical management of rape, having a positive impact on Syrians and Lebanese alike.

Lebanese mother Sally did not understand why her daughter was underweight. But after nutritional care was integrated within primary healthcare in Lebanon with funding from UNHCR, the three-year-old was successfully treated.
In addition, a total of 84 new specialized staff have been deployed by UNHCR and the International Organization for Migration to primary healthcare centers nationwide to accommodate increased demand for services.
Two years into the crisis, centres across Lebanon received post-exposure prophylaxis - special kits to help prevent HIV infection after a possible recent exposure. The counseling and treatment of survivors of sexual and gender-based violence (SGBV) has been institutionalized, and now includes psychological support and thorough case follow-ups.
Expanding care has also allowed medical teams to refer women and girls who survived SGBV to safe houses operated by specialized organizations such as UNHCR’s partner, the ABAAD-Resource Centre for Gender Equality.
Rola Hajj, director of nursing at the Tripoli Governmental Hospital, remembers a 17-year-old Lebanese girl rushing to the emergency room bruised from head to toe. Her parents had beaten her badly. They had forbidden her from leaving the house, even to attend school.
“That night she was received in one of the ‘women and girls safe spaces’ and has remained there since,” Rola said. Before its cooperation with non-profits like ABAAD, the Tripoli Governmental Hospital used to contact the police station when confronted with similar cases, having no recourse to specialized services.
In spite of these notable developments, Lebanon’s already fragile medical infrastructure has suffered with the arrival of a refugee population a quarter of its population’s size. Its highly privatized and expensive healthcare system continues to struggle with limited capacity that has been further eroded by the spike in needs.
“Hospitals and PHCs have been reeling under the weight of an additional million individuals who require urgent quality care. But a closer look at the impact of the refugee crisis reveals a lesser-known reality,” said Mireille Girard, UNHCR’s representative in Lebanon.
“People have more faith in public healthcare now. We hope to keep building on that.”
“Not only do Lebanese families have improved access to primary healthcare in a number of specialties, but many tell us they can now seek quality hospital care within their areas thanks to the introduction of much-needed equipment such as scanners, resuscitation equipment and incubators in hospitals across the country.”
The lack of modern equipment previously meant that Lebanese had to commute from remote areas to Beirut to access emergency hospital care.
“People have more faith in public healthcare now,” said Hamadeh. “We hope to keep building on that,” she added, noting that, with UNHCR, the Ministry has upgraded its information management system.
“The new, computerized database allows for the storage of each and every medical file and the tracking of individual cases in nearly half of the PHC network,” she said.
Another concrete example of progress: there are now 230 PHCs across Lebanon, an increase from 180 prior to the Syrian war.
Still, Hamadeh stresses the need for much more support. And she also worries about the sustainability of the new services. “We desperately need more funding,” she said. “We have come a long way, but gaps remain and we can’t be left alone at this point.”
* Names have been changed for protection reasons.