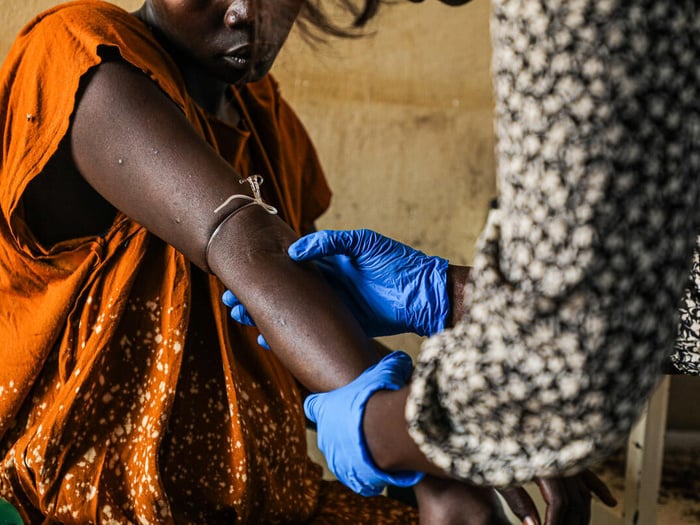
Access to healthcare
Access to healthcare
UNHCR works closely with national ministries of health and partner organizations so that refugees can get the health support and medical treatment they need in emergencies as well as in stabilized and protracted situations.

How does UNHCR help refugees get healthcare?
In all situations, UNHCR advocates for refugee inclusion in national health systems and plans. When appropriate, UNHCR provides technical guidance, supports infrastructure and capacity-building initiatives, as well as funding for human resources medicines, medical equipment and supplies.
Expanding access to health services for refugees often requires a combination of complementary interventions to strengthen national health systems and overcome financial barriers. UNHCR utilizes cash-based interventions to enhance access to health services by giving refugees the financial means to cover medical costs, including consultations, medications, and transportation. This flexibility empowers individuals to seek necessary care, reduces barriers to treatment, and improves health outcomes by promoting greater self-reliance.
If countries have or are planning to implement national social health protection schemes such as health insurance, UNHCR works with governments to advocate for the inclusion of refugees in such schemes.
Primary healthcare and referrals for secondary healthcare
Text and media 28
Primary healthcare practitioners provide support in the areas of sexual and reproductive health, nutrition, and child health including immunizations, mental health and the treatment of communicable and noncommunicable diseases. Primary healthcare practitioners also make referrals to secondary healthcare for a higher level of clinical care.
UNHCR improves primary healthcare for refugees and host communities by strengthening local health infrastructure (e.g. constructing or renovating facilities, providing medicines, medical equipment and laboratory diagnostics), funding and training health workers as well as supporting complementary health services during emergencies where national systems can’t be upscaled rapidly.
In addition, recognizing the needs of people with disability, UNHCR works with partners to facilitate access to assistive technology and rehabilitation.
Community health
Community health is a core component of the primary healthcare approach to prevent disease, promote well-being, and ensure equitable access to healthcare, fostering healthier, more resilient communities. Community engagement and participation are central to UNHCR’s approach, as they ensure that refugees have a voice in decisions affecting their health and well-being, fostering ownership, trust, and more effective, sustainable solutions to health challenges.
UNHCR trains refugee community health workers to engage with refugees, diagnosing and treating common illnesses (such as diarrhoea and malaria), making referrals and following up with pregnant women, newborns and people living with chronic diseases (e.g., diabetes and hypertension). Fluent in the languages and cultures of the refugee community, community health workers engage with the refugee community to share information about health, hygiene and preventative health measures such as immunization in ways that are culturally relevant and easily understood.
Noncommunicable diseases (NCDs) prevention and treatment
Noncommunicable diseases, such as heart disease, cancers, diabetes, chronic respiratory disease and mental health conditions, are the greatest source of preventable illness, disability, and mortality worldwide. Displacement can disrupt refugees’ treatment for these diseases or delay diagnosis, putting them at even greater risk.
In 2014, UNHCR began improving access to noncommunicable diseases care by ensuring that it is effectively integrated into primary healthcare. Through a capacity-building project, procurement of evidenced-based and cost-effective essential medicines and data collection and monitoring via the iRHIS (Integrated Refugee Health Information System), access to healthcare for noncommunicable diseases is now more systematically integrated into primary care services. UNHCR trains health staff on noncommunicable diseases care including screening, diagnosing and managing patients using clinical protocols (aligned with host country protocols). Capacity building includes training of staff to provide advice on smoking cessation, monitoring of disease control and awareness of complications.
Access to assistive technology, rehabilitation and related services
It is estimated that displaced populations have a higher proportion of people with impairments in functioning as well as injuries and a greater need for assistive technology and rehabilitative care. In addition, people may face barriers to accessing the required services or these may not be well established, and support is needed. Those in need may include:
- persons with disabilities such as long-term sensory or motor function loss ( e.g. requiring wheelchairs, hearing aids, visual acuity correction).
- people with short-term impairments or injuries; and people with chronic health conditions.
- women and girls with sexual and reproductive health-related conditions ( e.g. obstetric fistula and incontinence);
- older persons with reduced mobility.
Assistive technology and rehabilitation services overlap but are distinct. While some people will need to access both, other people will only need either one or the other.
UNHCR promotes inclusion in the national system if such services exist or enables access through partnerships with relevant organizations whilst aiming to build the capacity of national services. Multisectoral collaboration is required within UNHCR (health, community-based protection, education, settlement, shelter and WASH, development) as well as multi-stakeholder efforts working with governments and partners. Access at community and primary care level is promoted but higher level and more specialized services and referrals may be needed, where available.
UNHCR in partnership with WHO and partners has developed comprehensive guidance on assessing needs and promoting access to assistive technology and rehabilitative services for refugees.
Communicable diseases prevention and treatment
Text and media 29
Conflict and displacement that lead to refugee situations are a recognized public health risk. They increase the population’s vulnerability to communicable diseases because of weakened health systems, overcrowding, poor water and sanitation conditions, interrupted immunization activities and delayed diagnoses.
The main cause of death in many conflict and displacement situations is not violence, but the spread of communicable diseases such as malaria, measles and diarrhea.
UNHCR addresses the control of communicable diseases through a multisectoral approach, which includes enhancing access to vaccinations (especially against measles and polio) and improving access to water and sanitation facilities. Throughout all stages of refugee displacement, UNHCR prioritizes HIV and tuberculosis prevention and treatment. In addition, by utilizing the iRHIS system alongside community-based surveillance, UNHCR monitors conditions that have the potential to lead to communicable disease outbreaks.
Immunization
When refugees flee their homes, healthcare gets put on hold, including immunizations. As a result, refugees, especially children, are at increased risk of contracting vaccine-preventable diseases including measles, polio, viral hepatitis, diphtheria and whooping cough. Refugee children are also at very high risk of being “zero-dose” (no immunization) or under-immunized due to limited access to health services, lack of awareness or cultural barriers.
UNHCR promotes that all new refugee arrivals under 15 receive measles, polio and tetanus toxoid vaccines immediately. While vaccines are typically provided through ministries of health or UNICEF, UNHCR may need to support last-mile efforts to reach refugees UNHCR is identifying and addressing the needs of zero-dose refugee children, working closely with communities and local partners to identify and overcome key barriers to immunization in communities, including gender divides and the gap in demand and access.
Essential medicines, medical supplies and equipment
Text and media 33
Essential medicines are the medications considered to be most effective and safe to meet the most important health needs in a country. The World Health Organization (WHO) maintains a list of essential medicines that serve as a guide for states and institutions. Every two years, UNHCR reviews and adapts the WHO list for refugee contexts.
UNHCR procures and imports medicines from the UNHCR Essential Medicines and Medical Supplies list for emergency and ongoing refugee situations taking into account national essential medicine lists. These medicines are distributed through partners (including governments, national and international NGOs, and Red Cross/Red Crescent partners).
In emergencies, UNHCR also provides standardized medical kits (such as Interagency Health Kits, cholera kits, and reproductive health kits). The timely procurement and distribution of essential medicines and supplies are crucial in refugee settings, ensuring access to life-saving treatments for acute conditions and continuous care for chronic diseases.